Save 10% off on your first order with coupon code: FIRST
Buy Insulin Online From Canada
Humalog
Novolin
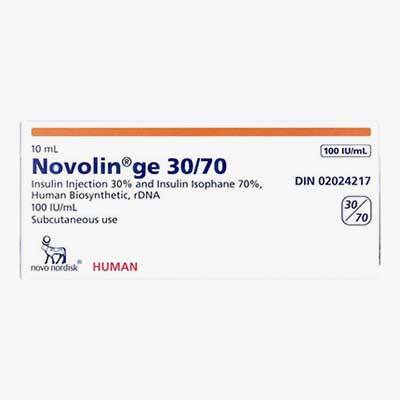
Novolin GE 30/70 Vial
(Insulin Injection, Insulin Isophane Human Biosynthetic)
30u/mL/70u/mL – 1 vial
$69
$194 (save 64%)

Novolin GE 30/70 Penfill Cartridge
(Insulin Injection, Insulin Isophane Human Biosynthetic)
30u/mL/70u/mL – 5 cartridges
$104
$344 (save 70%)
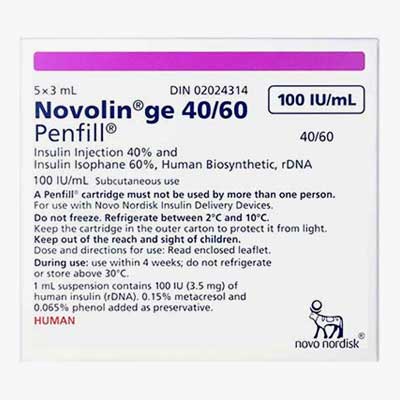
Novolin GE 40/60 Penfill Cartridge
(Insulin Injection, Insulin Isophane Human Biosynthetic)
40u/mL/60u/mL – 5 cartridges
$102
$344 (save 70%)
Novolin GE 50/50 Penfill Cartridge
(Insulin Injection, Insulin Isophane Human Biosynthetic)
50u/mL/50u/mL – 5 cartridges
$102
$344 (save 70%)
Other Insulin Brands
Frequently Asked Questions
Insulin is a natural hormone responsible for regulating blood sugar and many other processes in the human body. It’s produced by beta cells in the pancreas during digestion and helps body cells absorb glucose and turn it into energy. People with Diabetes either cannot produce insulin (Type 1) or don’t process it effectively (Type 2). For this reason, they need to take insulin in order to metabolize glucose.
Insulin works by moving glucose from your bloodstream into your body’s cells. It’s the agent that makes it possible for your cells to receive blood sugar (glucose) and turn it into energy for your body. Without insulin, glucose can’t enter your cells and builds up in your blood instead. This results in hyperglycemia (high blood sugar), which is one of the major concerns for people with Diabetes.
People take different types of insulin based on how quickly they need it to start acting and reach its peak (maximum) impact. Other factors include how long it lasts, how concentrated it is, and the method of delivery (subcutaneous injection, intravenous injection, or inhalation). Some common insulin types are:
- Rapid-Acting Insulin (begins working within 5-20 minutes and peaks 1-2 hours after injection)
- Regular/Short-Acting Insulin (begins working within 30 minutes and is effective for 3-6 hours)
- Intermediate-Acting Insulin (begins working within 2-4 hours and peaks after 4-12 hours later)
- Long-Acting Insulin (begins working several hours after injection and is effective for up to 24 hours)
- Ultra Long-Acting Insulin (begins working within 6 hours and lasts 36 hours or longer)
Patients with Type 1 Diabetes always require insulin. People with Type 2 Diabetes and other types of Diabetes may or may not require insulin on a regular basis. In certain circumstances, insulin may also be prescribed for patients suffering from other conditions (see Question 10 below).
Yes. Side effects are possible when taking insulin. Common side effects include swelling of the limbs and weight gain. Also common are injection site reactions (red, swollen, or itchy skin) and sometimes skin changes (such as shrinking or thickening).
Hypoglycemia (low blood sugar) can also occur if insulin intake isn’t properly regulated. Low blood sugar must be treated expediently. Symptoms include dizziness or lightheadedness, shakiness, hunger, blurred vision, slurred speech, high heart rate, and more.
Though rare, serious side effects of insulin can include severe hypoglycemia, low blood potassium, severe swelling of the hands and feet, cardiovascular events, and severe allergic reactions.
Insulin can have serious or moderate interactions with medications, including other Diabetes medications and even over-the-counter drugs. Your best source of information on how insulin may interact with specific medications will be your doctor or pharmacist.
The treatment of low blood sugar (hypoglycemia) usually involves the intake of sugary carbohydrates to bring blood sugar back up to normal levels. Consult your healthcare provider for a personalized treatment plan.
Yes. Less common clinical applications of insulin may include patients with septic shock and inflammatory conditions such as Crohn’s Disease, Rheumatoid Arthritis, Lupus, and some types of cancer.
Bisonpharmacy.com’s insulin products are primarily shipped from our partnered pharmacies in Manitoba, but can also be shipped from our partnered pharmacies in British Columbia.
No, it shouldn’t. Bisonpharmacy.com’s partnered pharmacies ship insulin in insulated containers with gel packs to ensure temperature control. In addition, insulin can be stored at room temperature for up to 30 days (but it’s best to refrigerate it as soon as your shipment arrives).
You can contact us directly toll-free with any questions at 1-888-668-2808.
Millions of Americans import drugs for personal use every single day. When ordering insulin from Bisonpharmacy.com, you must provide a prescription written by an American doctor and order no more than a 90-day supply at one time.
Manufacturers recommend refrigerating insulin, but it can also be stored for up to one month at room temperature. Never store insulin in extreme heat or cold. Avoid direct sunlight and check the expiration date as well as the appearance of the insulin prior to every injection.
Insulin that has expired or gone bad should be disposed of in a way that ensures it’s not attractive to children or animals. Consider mixing it with something unpleasant like coffee grounds and sealing it in a bag or container before putting it in the garbage. Always remember to remove your personal information from the packaging before throwing it away. Used needles or injectable pens must be properly disposed of in a medical-grade sharps container.
Yes. Canada’s highly regulated pharmaceutical industry makes it a safe country to import insulin from. Always be sure that you’re ordering from a high-quality, reputable service, such as Bisonpharmacy.com.